
Get to know our team on LinkedIN:
Dominique Rever Michaud, William Dunne, Betina Siopongco, Ramtin Doroodchi, Katie Vinterella
SNORELAX
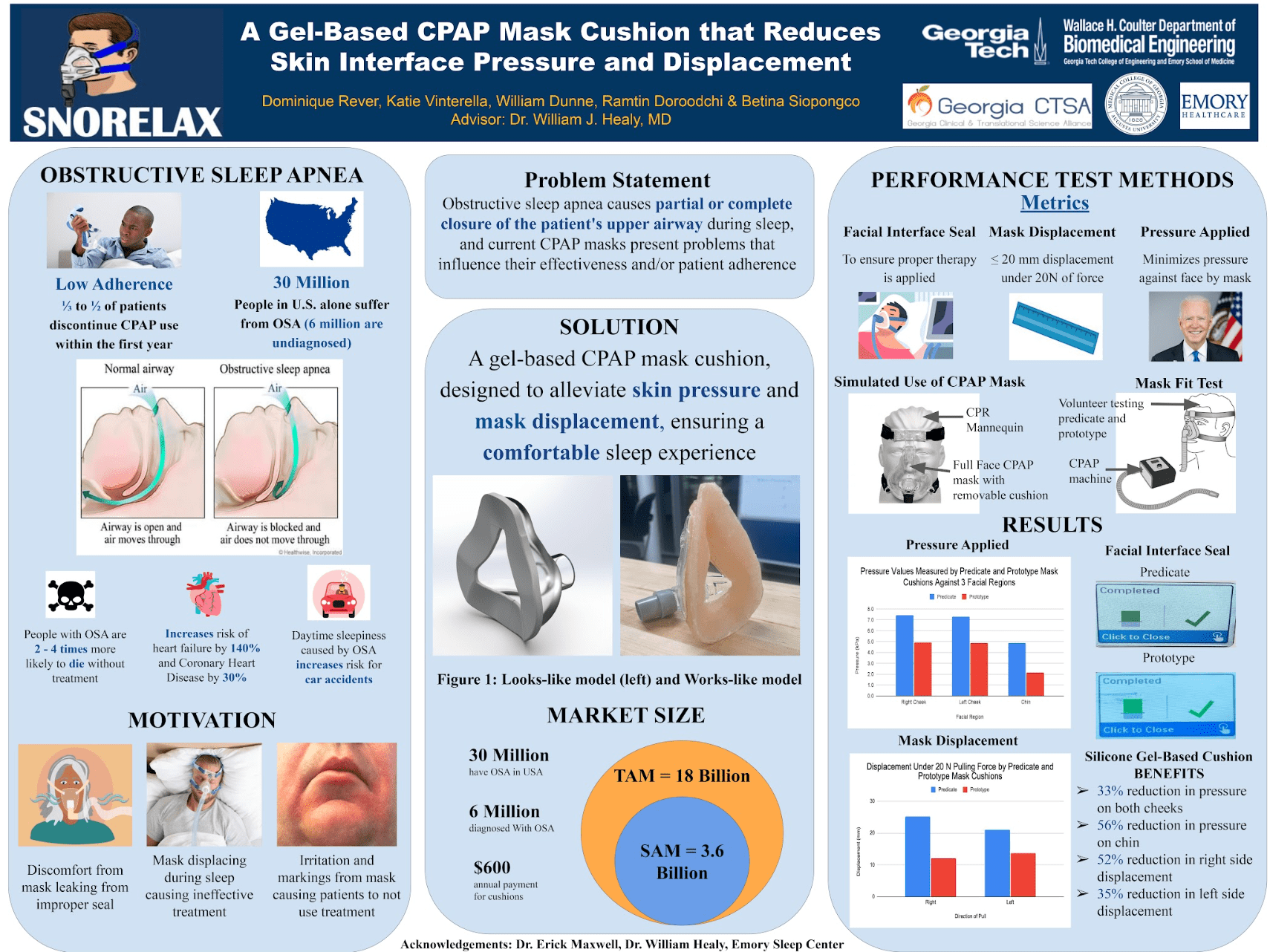
A Gel-Based CPAP Mask Cushion that Reduces Skin Interface Pressure and Displacement

Our prototype, pictured above, shows our Gel-Based CPAP Mask Cushion inserted in the CPAP mask frame featuring changes in facial interface material, area of facial interface, and the shape of the cushion as well. The facial interface material is now silicone-based gel, the area of facial interface has increased in order to decrease the pressure applied to each patient, and the shape increases sliding friction to reduce slipping. This can potentially lead to better patient adherence and increased comfortability.
Project Description:
Our project focused on developing an adaptive silicone gel-based CPAP mask cushion that molds to the face and increases the contact area to increase comfort and reduce the risk of slipping. Obstructive Sleep Apnea (OSA) is a disorder characterized by partial or full collapse of the upper airway during sleep. Continuous positive airway pressure (CPAP) devices, which administer pressurized air to keep the airway open, are the most effective and common therapy for OSA. Despite its effectiveness, patient adherence to CPAP therapy is low, with approximately 1/3 to 1/2 of patients discontinuing CPAP use within the first year. Commonly cited reasons for this low adherence include masks slipping off of the face, leaving potentially embarrassing red marks on the face in the morning, difficulty cleaning the mask, and incompatibility of masks with patients who have facial hair or uneven facial topography. To address these challenges, we created a gel-based, full-face CPAP mask cushion. It utilizes a double gel-based layer material made out of silicone gel. The silicone gel layer increases the area of contact with the patient’s face compared to other mask cushions. This increased area allows for a better distribution of the pressure against the facial skin from the mask straps, which reduces the risk of developing red marks on the facial skin. This increased contact area also creates friction between the cushion and face, which reduces the amount that the mask slips if force is applied to it, and helps the patient keep the mask against their face even if they are moving in their sleep. The double layer improves the fit and aids in the distribution of the pressure against the face. Our solution would increase patient adherence to their prescribed treatment and lessen the chances of patients developing complications from OSA such as cardiovascular issues.

Dr. William J. Healy, MD
Division of Pulmonary, Critical Care, and Sleep Medicine, Department of Medicine, Medical College of Georgia at Augusta University
